Workers in the UK who are ‘economically inactive’ now number 600,000 – a population roughly equal to a city the size of Manchester, who could be working but feel that they are unable to. A large contingent, particularly towards the younger end of this group, are reporting ill heath due to stress, anxiety and depression. The question needs to be asked, rather than their sickness being the thing that’s preventing them from working, is work the thing that’s making them sick?
Of course, it would not be the first time that people’s occupations have been hazardous to their health. You don’t even need to look that far back to find whole industries where risk of death was routinely accepted as part of the job. Yet huge progress was made in the 20th century to reduce work-related fatalities – from 61 workers in 100,000 dying at work at the beginning of the century, to 3.2 by the end – a 95% reduction. [i]
Yet this physical danger has been replaced, possibly even surpassed, by psychological danger. Sarah O’Connor of the FT puts this rising psychological cost down to a particularly toxic combination of the intensification of work (the pressure to work harder and faster) coupled with less autonomy, particularly among the lower paid. Between 1992 and 2017, the share of low-paid workers who report that they have a say in decisions which affect their work fell from 44 per cent to 27 per cent.[ii] It is important to note here that there is a proven link between shift work, particularly at night, and often a feature of the lower paid professions, and ill health.
So, sure, you may not pay the ultimate price of death for going about your day-to-day work these days, but the insidious and gradually debilitating effects of long-term poor mental health on the individual, not to mention impact on the NHS and cost to the economy, are not to be underestimated.
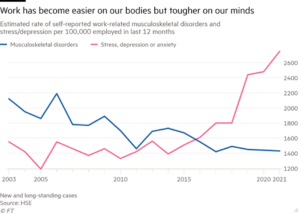
This trend of increasing work-related stress, depression and anxiety predates COVID-19 (see graph, below) and then accelerated during the pandemic itself, but as we enter the post-pandemic era of work, might there be some hope that things could change – namely, with flexible working? Unfortunately, that case is not clear cut, either. Yes, flexible working practices (such as, greater choice around hours and work locations) can improve both mental and physical health, but only when guided by a clear, supportive framework.[iii]
So will big business take up the gauntlet? Perhaps before they announce their new yoga series at lunch or mental health helpline, they could first interrogate their flexible working policies – many of which are still a patchwork of hastily arranged, informal agreements made during the pandemic – and put in place a structure which fundamentally hands back some control over where and when they do their work, back to employees.
[1] Steven Pinker, “Enlightenment Now: The Case for Reason, Science, Humanism, and Progress,” 2018
[2]Sarah O’Connor, “What if work is making us sick?”, Financial Times, 22nd Dec 2022
[3] Flexible work supports mental wellbeing, but only good leadership
https://www.swinburne.edu.au/news/2022/11/flexible-work-supports-mental-wellbeing-but-only-with-good-leadership/
